Whirika Maimoataka
Treatment Options
Taking care of your shoulder pain
Most shoulder pain gets better naturally over time but that can take several months. Flare-ups or setbacks can happen – we are all human!
On this page, we cover the following:
Reasons for seeking healthcare urgently for shoulder pain
Specific treatment for a new shoulder injury
General advice for shoulder pain
Sleeping tips
Generic overview of what health professionals and treatment providers can offer.
We specify the individual provider's roles more clearly under ‘Finding a health provider’.
Reasons for seeking health care urgently for shoulder pain
You should see your GP, urgent doctor, physiotherapist or other health care professional if any of the following applies:
The pain is getting worse rather than better, despite following self-management or initial pain medication
Possibility of a fracture or dislocation (attend A&E or Urgent Doctors if you suspect a fracture or dislocation)
Unable to lift the arm
You have pain at night, possibly worse than during that day, that prevents you from sleeping
Tingling (pins and needles), numbness or burning feeling in the arm, hand or fingers
Blueness or cold feeling in the arm, hand or fingers
The joint is becoming hot and swollen
You feel unwell, and have symptoms such as a fever, night sweats or weight loss.
Specific treatment for a new shoulder injury
After an injury you may have to limit specific movements to allow pain to settle. Listen to your body in terms of what to avoid.
Pain medication may be useful. Consult a pharmacist or your GP.
Ice or heat over the area may be useful in the acute stage, although the research evidence is low. If you find ice or heat helpful, continue to use it to settle down the pain.
If your shoulder was disclocated, you may be prescribed a sling in the early recovery period. Wean yourself off the sling as advised by the health provider.
Do gentle exercises for the shoulder as soon as is possible, monitoring your pain. It is OK to feel some pain during the exercise, but that should settle down after the exercises. See ‘Helpful exercises’.
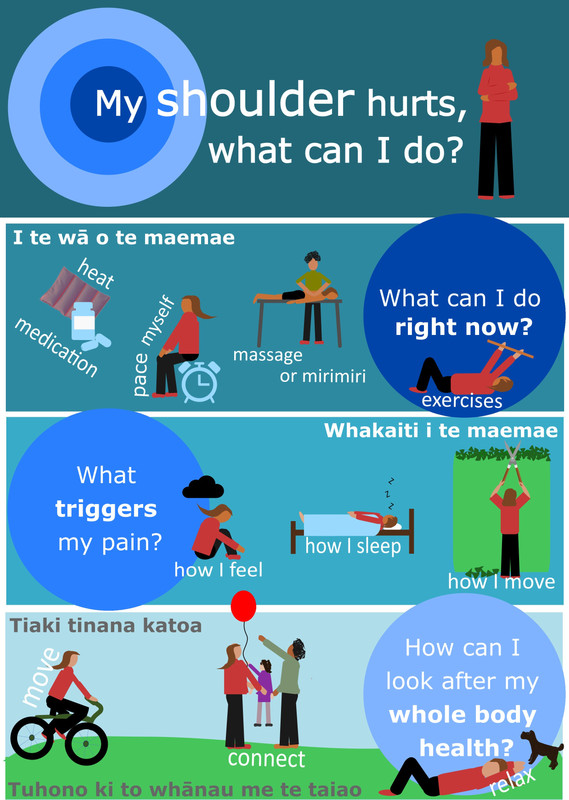
General advice for shoulder pain
We need to think ‘beyond the shoulder’ to take care of your shoulder pain. We need to consider your ‘whole body whānau’. Considering the brain as a ‘super-computer’, we need to do things that bring the brain and nervous system into 'low alert'.
Work out what relieves your shoulder pain. People respond differently to treatments. What helps you depends on many things, including your lifestyle - your daily tasks, work, hobbies, sports and exercise - and your beliefs. Try to find out what relieves your pain, for example specific movements or postures. Take note of whether your pain gets worse when you are feeling stressed out, anxious about things, or when you just have too much to do. In the early phase of your pain or when you have a flare-up, minimise the movements that make the pain worse.
Pacing. Pacing means that you 'chunk' tasks into shorter time periods, alternated with rest or doing other tasks. See more information under FAQs.
Keep active. That may entail going for regular walks, in a ‘green space’ if possible, on the beach, or around the block. Stay connected with your sports team or mates; join community group classes for motivation and to connect with others.
Do things that make you feel positive. Feeling down and frustrated is understandable when we have pain and stiffness. Connect with whānau, friends, or colleagues on a regular basis, or spend time alone doing something you enjoy.
Sleep care. See tips below.
Take care of your health. If you are living with a long-term condition (for example diabetes or high blood pressure), follow advice provided by your GP.
Look after your weight. Consider what you eat and drink. Ask your GP for a referral to get advice from a dietitian or nutritionist, if necessary.
Take control of smoking and excessive alcohol habits. People who smoke generally take longer to recover from injuries and pain.
In the workplace. Talk with your employer or line manager about your pain. Ask if an occupational health nurse or physiotherapist is available to provide advice about your working-related posture and movements. There is no ‘one correct posture’, so work with them to find out what is best for you. You can also ask your health care provider for support to liaise with your employer.
Sports and recreation. Doing too much or too little, or not having enough time to recover between intense training or activity sessions may contribute towards shoulder pain. How we perform repetitive movements (for example swimming, rowing or golf stroke) may also influence the pain. Work with a coach or physiotherapist to consider how training could be modified. Return to full training and competition should be gradual and progressive (staged).
Tips for sleeping
When lying on the opposite (painfree shoulder), try using a pillow in front of you to rest the sore arm on. Alternatively, use a small pillow or towel between your chest and the upper arm to rest the arm on.
Try sleeping in a semi-turned position when lying on your back, with a pillow under the side of your injured side. Placing a pillow under your knees may help you to relax.
Some people with shoulder pain may find it helpful to sleep in a seated position with the sore arm supported by pillows during some nights.
Choose a mattress that is of medium hardness: not too soft or too hard. If it is starting to sag at places, consider buying a new one, if possible. Turning the mattress around regularly will increase its durability.
Avoid strong lights and blue light (TV, computers, mobile phones) at least 30 minutes before bedtime.
Have a night-time routine. Have regular times for getting to bed and for getting up in the morning, if possible.
Having a warm drink before going to bed may be helpful.
Read a book or listen to gentle music to help you relax.
Have a quiet time. Many people find it helpful to pray, meditate or practice mindfulness.
Have a pen and writing pad next your bed. If you wake up with worrying thoughts, write them down and consider them the following day.
If pain keeps you awake at night, talk to your GP for options for pain medication. Ask for information for how long (how many days) you may take those medication. Wean yourself off the medication as soon possible.
What health providers can offer
Korero (conversation). They will work with you to find out what the problem is and what works for you. They will help you to find out what you can do yourself to take care of your shoulder pain, how to minimise flare-ups, and what you can do if you have a flare-up. They should provide information and advice that is relevant for you and your whānau, and answer your questions.
Assess your shoulder pain and how it affects you. If you have had an injury, they may open a claim for the Accident Compensation Corporation (ACC). The clinician should find out with you if there are other reasons why you have shoulder pain.
Help with decision about pain medication. A GP or pharmacist may prescribe pain medication, advise you how much you should take and for how long it is safe to take. For rotator cuff related shoulder pain, a corticosteroid injection may be helpful for the short term. For frozen shoulder, a corticosteroid injection may also be useful in the early painful phase.
Exercise prescription. Specific exercises for your shoulder will form the main part of your recovery. Your health provider should work with you to find out what exercises are best for you, and also which exercises you prefer. See ‘Helpful Exercises’.
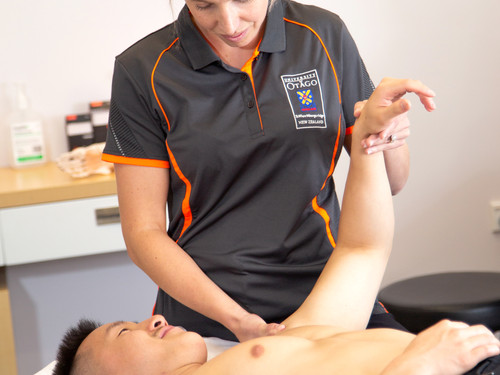
Manual therapy, massage. The research evidence about manual therapy or massage indicates that it can be useful for pain relief in the short term when included as part of a wider treatment. By itself, manual therapy is unlikely to help the recovery. Physiotherapists and osteopaths may apply manual therapy or massage techniques, and re-assess what benefit it has for you. They would most likely use manual therapy and massage as an addition to exercise rehabilitation.
Miri miri is a Māori holistic healing tradition that includes massage techniques. That treatment includes physical and spiritual elements and can form part of recovery.
Acupuncture. Some physiotherapists and other health providers offer acupuncture or needling for pain relief, particularly for acute pain. Interpreting research evidence, it is more likely that acupuncture can be used for pain relief in combination with physiotherapy and exercise, rather than as a standalone treatment.
Refer you for investigations if needed. An X-ray, ultrasound or MRI may be considered if there is a specific reason and if the results will inform your path to recovery.
Help with decisions about surgery. In some cases, surgery may be considered if the pain does not improve or is getting worse. If you have dislocated your shoulder and it keeps on happening again, surgery may be considered.
Help with decisions about referrals to other health care provider. If your pain is persistent, the clinician may consider with you whether you and your whānau should be referred to an orthopaedic surgeon, a pain clinic, or other healthcare provider.
Support you get active or get back to your preferred activities. The health provider should explore with you what physical activities you prefer and devise a progressive plan to enhance your physical activity.
Provide support and advice for adjusting work-related tasks, if necessary. If your shoulder injury is work-related, an occupational health nurse, physiotherapist or occupational therapist (OT) can provide advice for the required tasks you need to complete. That may entail advocating for adaptive equipment, technology or manageing your workload. If you need time off work because of your shoulder pain, your GP would need to provide supporting documentation.
Provide guidance for return to sport and recreation. Physiotherapists provide guidance for return to sport and recreation, devising a programme or strategies that are relevant for you. In some instances you may need to consider changeing to another sports, for example, if your shoulder injury recurs frequently despite rehabilitation. The physiotherapist can provide support for considering those decisions and options. A mental skills coach may also be available to support you with gaining confidence when returning to sports and activity or when considering a change in sports.
Infographic by Ihaiah Kendrick, HRC Māori Summer Studentship, December 2023/January 2024.
Page checked by Gisela Sole, 25th September 2025.